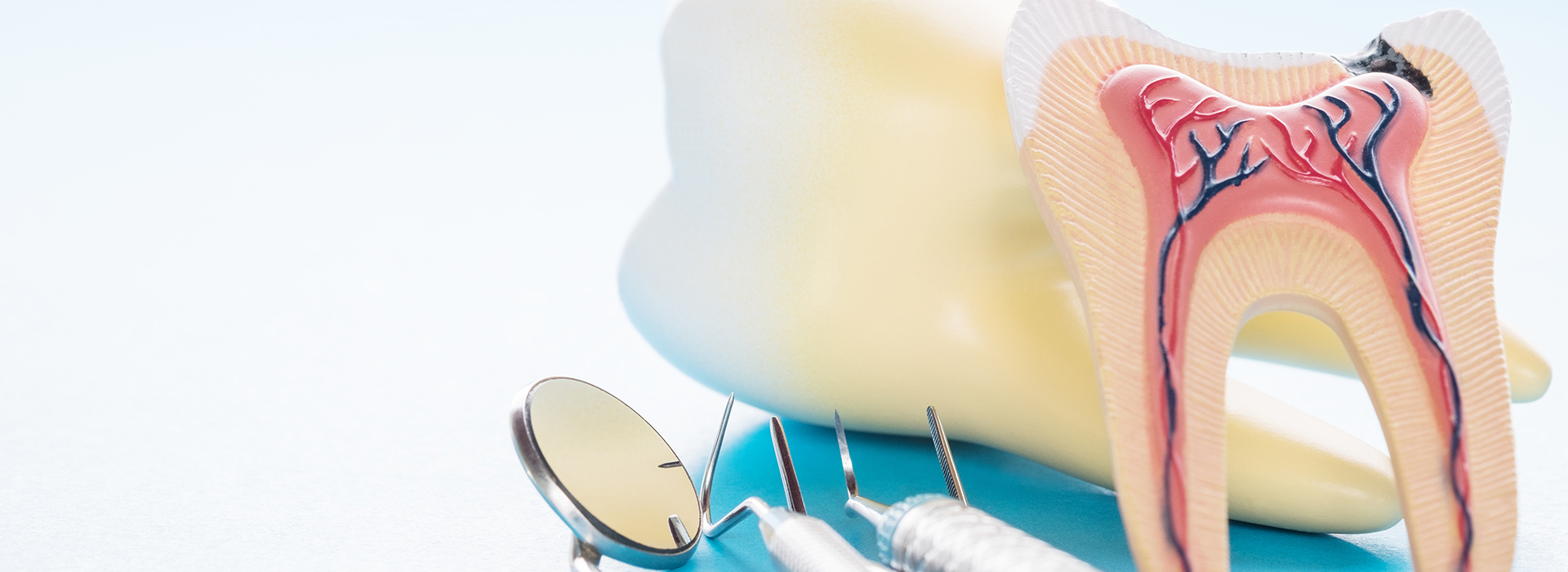
If your dentist recommends a root canal, take a breath — this treatment is focused on relief, preservation, and restoring function rather than fear. Modern root canal therapy is a precise, minimally invasive way to remove inflamed or infected tissue from the center of a tooth, relieve pain, and retain the strength and appearance of your natural smile.
Our team approaches each case with careful diagnostics and patient comfort in mind. At Bella Vida Dental, we combine up-to-date techniques with attentive care so patients understand what’s happening and feel supported throughout the process.
When a tooth’s inner tissues — the pulp — become damaged by decay, trauma, or infection, the structural integrity and long-term viability of the tooth can be at risk. Root canal therapy is designed to remove the diseased tissue, disinfect the internal spaces, and seal the canals to prevent reinfection. By preserving the existing tooth, you avoid the functional and aesthetic compromises that can follow extraction.
Beyond aesthetics, keeping a natural tooth helps maintain proper chewing function and prevents adjacent teeth from shifting. Restoring the treated tooth with a crown or other suitable restoration further reinforces it against fracture and wear, returning the tooth to dependable performance for daily activities like eating and speaking.
Advances in instrumentation, imaging, and materials have made the procedure more predictable and comfortable than ever. While individual cases differ, many treated teeth go on to serve patients well for years when combined with good oral hygiene and routine dental care.

Not every sensitive or aching tooth requires a root canal, but several warning signs merit prompt evaluation. Persistent, deep pain that lingers or wakes you at night often signals irritation of the nerve tissues. Likewise, heightened sensitivity to hot or cold that does not subside after the stimulus is removed can indicate pulpal inflammation.
Changes in the appearance of a tooth — such as darkening or discoloration after an injury — may reflect internal tissue changes that deserve assessment. Pain when biting or tenderness to touch can point to nerve involvement or a developing infection. Gum swelling or a small pimple-like bump near a tooth root can signal an abscess that requires prompt care.
If a tooth feels loose or if discomfort persists despite home care, it’s important to seek an examination. Digital X-rays and clinical tests help determine whether the pulp is compromised and whether root canal therapy or an alternative approach will best protect your oral health.
Delaying evaluation or treatment when the pulp has been damaged can allow infection to spread, potentially affecting surrounding bone and soft tissues. Early intervention frequently limits the extent of treatment needed and reduces the chance of more complex procedures later on. In some cases a tooth with little visible damage may show changes on a radiograph before symptoms arise, which is why routine dental exams are so valuable.
Addressing pulpal disease in a timely way also minimizes discomfort, helps preserve supporting bone, and improves the odds of a long-term successful outcome. If infection is already present, treating it promptly reduces the risk of more widespread oral or systemic effects and supports faster, more predictable healing.
Your dentist will weigh factors such as remaining tooth structure, the extent of infection, and overall oral health when recommending the best course of action. Acting sooner rather than later helps protect surrounding teeth and keeps future restorative options broader and more conservative.
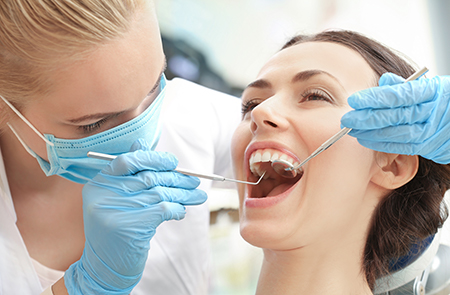
A typical root canal appointment begins with careful numbing of the area so patients remain comfortable throughout the procedure. Using magnification and modern instruments, the dentist gains access to the interior of the tooth, removes the diseased pulp, and mechanically and chemically cleans the canal system to eliminate bacteria and debris.
Canal anatomy varies by tooth; some treatments are completed in a single visit, while others may require two appointments when infection, anatomy, or restorative needs dictate. Once the internal spaces are prepared and disinfected, the canals are filled with a biocompatible material and sealed to reduce the chance of reinfection.
To address anxiety or increased comfort needs, sedation options are available and can be discussed with your clinician. Following canal treatment, a temporary restoration is often placed until a permanent crown or other restoration can be completed to restore strength and function.
After the procedure, mild sensitivity and soreness are common as surrounding tissues heal; these symptoms typically subside over a few days. Over-the-counter pain relief is usually effective, and when indicated, your dentist may prescribe medications to address infection or more significant discomfort. It’s important to follow any medication instructions and complete a prescribed antibiotic course if one is given.
A tooth that has undergone root canal therapy remains more brittle than an untreated tooth, so restoring it with a crown or an appropriate permanent restoration is an important step to prevent fracture. While waiting for the final restoration, avoid chewing hard or sticky foods on the treated side and maintain careful oral hygiene to support healing.
With attentive restorations and routine dental checkups, a treated tooth can function well for many years. If you notice renewed pain, swelling, or any unexpected change following treatment, contact the dental team promptly so the situation can be evaluated and addressed.
In summary, root canal therapy is a reliable option for relieving pain, controlling infection, and preserving natural teeth whenever the pulp has been compromised. The procedure is performed with comfort and precision in mind, followed by restorations designed to return the tooth to long-term function.
If you have questions about root canal treatment or think you may need an evaluation, please contact us for more information.

A root canal procedure is the best way to save a tooth that has been damaged by decay or injury and preserve your natural smile. The alternative is an extraction and treatment to replace the tooth. While at times a tooth is non-restorable and an extraction is the only option, when possible, it’s best to try and save your natural tooth. With proper care, a tooth with root canal therapy can serve your smile well for many years to come.
Despite lingering myths from before the age of modern dental anesthesia and technology, having a root canal procedure today is as routine and comfortable as visiting the dentist for a filling. While the procedure is performed under local anesthesia with your tooth completely numbed, we can also discuss options in dental sedation.
Whether the symptoms of a dental infection subside after a course of antibiotics, a draining abscess provides you with some temporary pain relief, or a tooth with radiographic evidence of pathology has not yet developed symptoms, it’s essential, before an infection worsens or occurs, to have a root canal procedure performed. In this way, the tooth can be disinfected, filled, and sealed to protect your health and avoid further problems.
If you have sustained a dental injury, have a toothache, jaw pain, swelling, or are experiencing any other unusual and uncomfortable oral symptoms, contact our office immediately for care. Dental problems that have not been evaluated and treated can significantly worsen, producing more severe damage and consequences for the involved teeth, your oral health, and even your overall wellbeing. Once you get in touch with our office, our friendly and compassionate office team will get you in for care at your earliest convenience.
While some root canal procedures can be completed in one visit, others may involve 2 or 3 appointments. How long it takes depends on various factors, including active infection, the number of canals in the tooth, and the tooth’s location or anatomy.
With a success rate that exceeds 95%, root canal therapy remains the most effective procedure to save a tooth in which the inner vital tissues have been damaged. However, as with all healthcare procedures, there are a small percentage of cases where the teeth become symptomatic a second time. The good news is that many of these teeth can still be saved with root canal retreatment or a minor surgical procedure known as an apicoectomy.
The best ways to maintain a tooth with root canal therapy are to get the proper restoration required to rebuild and protect the tooth, maintain proper oral hygiene, and schedule appointments for routine dental checkups and care.
Saving a tooth with root canal therapy is a wise investment that, in the long run, is typically less costly and invasive than having the tooth extracted and replaced with a fixed bridge or implant. As far as the exact cost of care, it can vary depending on which tooth is being treated. Many dental insurance plans provide coverage for root canal therapy. At the office of Bella Vida Dental, we do our best to optimize your dental benefits and minimize your out-of-pocket expenses. Our staff will answer all your questions about the cost of care and discuss all your payment options.
At the office of Bella Vida Dental, we use the latest technology and most effective methods of care to provide precise and gentle care. Our reputation for excellence is based upon a consistent record of achieving successful treatment outcomes while providing prompt, stress-free, and convenient treatment for every type of dental need.
A root canal is a dental procedure that removes inflamed or infected tissue from the center of a tooth to relieve pain and prevent further infection. The treatment focuses on cleaning, disinfecting, and sealing the internal canal system while preserving the natural tooth structure. By retaining the tooth, root canal therapy helps maintain chewing function and facial structure.
Diagnosis and treatment planning rely on clinical exams and imaging to assess the extent of pulp damage and surrounding bone. At Bella Vida Dental in Tucson, clinicians combine magnification, modern instruments and sterilization protocols to make the procedure predictable and comfortable. When appropriate, sedation options are available to help patients remain relaxed during treatment.
Common signs that a tooth may need a root canal include persistent or severe toothache, especially pain that lingers or wakes you at night. Heightened sensitivity to hot or cold that does not subside after the stimulus is removed is another frequent indicator. Visible changes such as darkening of a tooth, swelling of the gums, or a small bump near the root may also signal pulp disease.
Not all sensitivity means root canal therapy is necessary, so clinicians use digital X-rays and clinical tests to evaluate pulp vitality and infection. These diagnostic tools help determine whether the nerve is inflamed, necrotic, or if an abscess has formed. Early assessment often allows for more conservative care and better long-term outcomes.
Treatment begins with local anesthesia to numb the tooth and surrounding tissues so patients remain comfortable during the procedure. A small opening is made in the tooth to access the pulp chamber and root canals, after which debris and infected tissue are removed. The dentist cleans and shapes the canal system using mechanical and chemical methods to eliminate bacteria and reduce the risk of reinfection. Magnification and modern instruments improve precision and efficiency throughout these steps.
Once cleaned, canals are filled with a biocompatible material and sealed to prevent bacterial ingress, and a temporary restoration is placed when needed. Some cases are completed in a single visit while others require two appointments depending on infection severity or anatomy. A final restoration, typically a crown, is recommended to reinforce the treated tooth against fracture.
Thanks to contemporary anesthetic techniques and advances in operative methods, most patients experience minimal pain during a root canal procedure. Dentists also offer sedation options for patients with dental anxiety or complex needs to enhance comfort and reduce stress. Communication about sensations during treatment helps the dental team adjust anesthesia and ensure a tolerable experience.
After the procedure, it is common to feel mild soreness or sensitivity as surrounding tissues heal, which typically resolves in a few days. Over-the-counter pain relievers are often sufficient, and your clinician will provide guidance if additional medication is needed. If severe or worsening pain, swelling, or fever occurs, contact Bella Vida Dental promptly so the team can evaluate and address the issue.
Short-term recovery usually involves minor soreness around the treated tooth and gum that improves over several days with rest and gentle oral hygiene. Patients are advised to avoid chewing hard or sticky foods on the treated side until the final restoration is placed. Following any prescribed medications and the clinician’s post-operative instructions supports uncomplicated healing.
A permanent restoration, such as a crown, is often recommended to restore strength and prevent fracture, and scheduling this restoration is an important part of long-term success. Regular dental checkups and good home care help monitor the treated tooth and detect any changes early. If symptoms return or new concerns arise, prompt re-evaluation improves the chance of a successful resolution.
A tooth that has undergone root canal therapy can last many years or a lifetime when it is properly restored and maintained. Factors such as remaining tooth structure, the quality of the restoration, oral hygiene, and bite forces influence its longevity. Routine exams and hygiene visits allow clinicians to assess restorations and address issues before they compromise the tooth.
In some cases a previously treated tooth may require retreatment or surgical endodontic procedures if symptoms reappear or radiographs show persistent infection. These options can often preserve the tooth without extraction when performed by experienced clinicians. Discussion of risks, benefits, and expected outcomes helps guide decisions tailored to each patient’s situation.
Preserving a natural tooth with root canal therapy generally maintains chewing efficiency, prevents neighboring teeth from shifting, and preserves jawbone support. Saving the tooth also simplifies certain restorative and prosthetic planning compared with extraction and replacement. Whenever feasible, clinicians prioritize treatments that retain healthy tooth structure while eliminating infection.
However, extraction may be necessary when a tooth is nonrestorable due to extensive damage, severe periodontal disease, or vertical root fracture. When extraction is recommended, replacement options such as dental implants or bridges are considered to restore function and appearance. A thoughtful evaluation balances long-term oral health, the condition of surrounding tissues, and the patient’s overall needs.
Accurate diagnosis starts with a thorough clinical exam, patient history, and diagnostic tests that may include digital X-rays and, when indicated, CBCT imaging to view complex root anatomy. CBCT provides three-dimensional detail that is valuable for assessing root morphology, nearby structures, and the extent of infection. These imaging tools help clinicians plan treatment strategies and anticipate potential challenges.
Additional tests such as cold or electric pulp testing, percussion, and mobility assessment contribute information about nerve health and the tooth’s prognosis. Combining clinical findings with imaging results gives a comprehensive picture for informed decision-making. This approach reduces surprises during treatment and supports predictable outcomes.
Not every damaged or infected tooth is a candidate for root canal therapy; alternatives include watchful waiting with regular monitoring in asymptomatic cases or extraction when the tooth cannot be restored. Antibiotics may be prescribed temporarily when infection is present, but they do not resolve the underlying pulp problem and are not a standalone solution. When extraction is chosen, clinicians discuss appropriate replacement options to restore function and prevent long-term complications.
The choice between treatment options depends on factors such as the tooth’s structural integrity, periodontal health, patient preferences, and overall oral health goals. A conservative approach that preserves natural teeth is commonly favored when it offers a reliable prognosis. A clear explanation of risks and benefits helps patients make informed choices aligned with their priorities.
Before your appointment, provide a complete medical and dental history and let the team know about medications or medical conditions that could affect treatment. If you plan to use sedation, follow the clinician’s pre-procedure instructions regarding eating, drinking, and transportation. Adequate rest and light meals can help you feel more comfortable during the visit.
Arrive with a list of questions or concerns so the dentist can review the treatment plan and expected steps with you beforehand. Bring any recent dental records or radiographs if available to support assessment and continuity of care. Understanding the anticipated timeline for restoration and follow-up visits ensures the best chance for a successful outcome.

Ready to schedule your next dental appointment or have questions about our services?
Contacting Bella Vida Dental is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.