Temporomandibular joint disorders (TMJ or TMD) affect millions of people and often present as persistent discomfort around the jaw, face, or ears. While occasional jaw stiffness is common, a true TMJ disorder is a functional problem involving the joints, muscles, or connective tissues that control jaw movement. Understanding what contributes to these conditions and how they are evaluated helps patients take informed steps toward lasting relief.
TMJ disorders can arise from a variety of sources and rarely have a single cause. For some people, a history of teeth grinding (bruxism), a jaw injury, or chronic strain from chewing and clenching sets the stage for persistent symptoms. Others develop joint changes related to arthritis or long-term stress, which alters muscle tension and joint mechanics over time.
Certain lifestyle and health factors increase the likelihood of developing TMJ problems. Repetitive habits like chewing gum, nail-biting, or frequent yawning, poor posture that affects neck and jaw alignment, and untreated sleep-related breathing disorders can all contribute. While TMJ disorders can affect any age group, they are most commonly diagnosed in adults and tend to be more prevalent among women.
Because TMJ conditions can present differently from person to person, a tailored approach to evaluation and care is important. Early recognition of symptoms and prompt consultation with a dental professional can prevent minor jaw discomfort from becoming a more persistent, limiting issue.
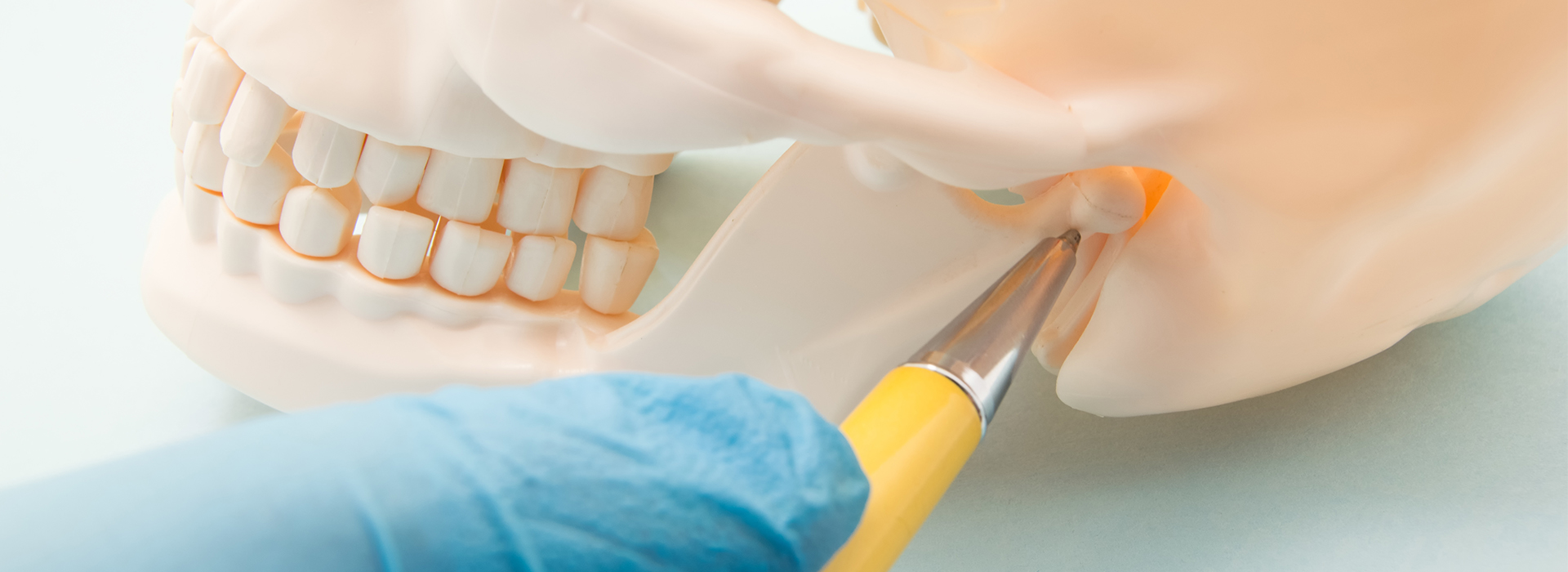
The temporomandibular joint is a paired joint—one on each side of the head—that connects the lower jaw (mandible) to the temporal bone of the skull. Unlike simple hinge joints, the TMJ allows a combination of hinge and sliding motions that enable chewing, speaking, yawning, and facial expressions. This versatility makes the joint uniquely prone to complex patterns of wear and strain.
A small, fibrous disc sits between the moving parts of the joint and acts as a shock absorber and a stabilizer. Muscles, tendons, and ligaments surround the joint and coordinate its movement. Disruption to any component—disc displacement, muscle imbalance, or inflammation—can interfere with normal motion and produce pain, sounds, or locking.
Because the joint works in concert with muscles of the face, neck, and upper shoulders, dysfunction in one area often affects the others. That interconnection is why TMJ care frequently involves collaboration between dentists, physical therapists, and sometimes medical specialists to restore comfortable, efficient movement.
Many people associate TMJ disorders with a single event, but often several contributing factors overlap. Teeth grinding or clenching is among the most common triggers—especially when it occurs during sleep—because it places repetitive stress on the joint and surrounding muscles. Trauma from a direct blow or a dental procedure can also precipitate symptoms.
Systemic conditions, such as rheumatoid arthritis or osteoarthritis, may directly affect the joint surfaces and lead to progressive changes. Additionally, emotional and physical stress can increase muscle tension and promote parafunctional habits (unconscious muscle activity) that perpetuate pain and dysfunction.
Even dental problems that alter bite relationships—worn restorations or missing teeth—can change the way the jaw aligns and moves. Part of a comprehensive evaluation is identifying and addressing these interrelated factors so that treatment targets the true drivers of a patient's symptoms.
TMJ-related complaints vary widely, but several patterns frequently appear. Jaw pain or tenderness, especially when chewing or opening wide, is often the first symptom patients notice. Clicks, pops, or grating sounds during jaw movement may indicate disc displacement or altered joint mechanics, while episodes of jaw locking suggest a mechanical obstruction or severe muscle spasm.
TMJ disorders can also produce symptoms that seem unrelated to the jaw itself. Headaches—particularly in the temples or at the base of the skull—ear discomfort or a sensation of fullness, and dizziness or ringing in the ears are commonly reported. These complaints can make diagnosis challenging without a careful, focused clinical assessment.
Limitations in how wide the mouth opens, difficulty biting or chewing certain foods, and increased facial or neck muscle fatigue are additional clues. If symptoms interfere with sleep, work, or daily routines, seeking an evaluation is advised rather than waiting for spontaneous resolution.
Diagnosis starts with a thorough history and clinical exam to identify pain patterns, jaw motion limits, and associated muscle tenderness. Dentists may observe the way teeth fit together, listen for joint sounds, and assess muscle function. When needed, imaging such as cone-beam computed tomography (CBCT) or magnetic resonance imaging (MRI) provides detailed views of bone, joint spaces, and soft tissues to guide care decisions.
Treatment typically begins with conservative, reversible strategies aimed at reducing pain and restoring normal function. These may include behavioral changes (reducing chewing of hard foods, avoiding gum), targeted jaw-stretching and relaxation exercises, and short-term use of over-the-counter anti-inflammatory medications as appropriate. Night guards or stabilization splints can protect teeth and reduce clenching-related stress on the joint.
For persistent or more complex conditions, additional therapies are available. Physical therapy focused on the jaw, neck, and shoulders can improve posture and muscle balance. Interventional options—such as corticosteroid injections, Botox® in selected cases, or occlusal adjustments—are considered when conservative measures are not sufficient. Orthodontic or prosthetic treatments can correct bite relationships when they contribute to dysfunction. Surgical approaches are reserved for structural problems that do not respond to non-surgical care and are pursued only after careful multidisciplinary evaluation.
Successful management depends on an individualized plan that addresses the root causes, not just the symptoms. Ongoing monitoring, patient education, and coordination among care providers help ensure steady improvement and reduce the chance of recurrence.
At the office of Bella Vida Dental, we approach TMJ concerns with a focus on clear explanations, evidence-based options, and personalized strategies that prioritize comfort and function. If you suspect a TMJ disorder or have persistent jaw-related symptoms, an early assessment can help determine the most appropriate path forward.
In summary, TMJ disorders encompass a range of conditions affecting the jaw joint and its supporting structures. Although symptoms can be varied and sometimes puzzling, careful evaluation and a stepwise treatment approach provide effective relief for most patients. Contact us for more information about TMJ care and to discuss an evaluation tailored to your needs.

TMJ disorders are a group of conditions that affect the temporomandibular joints, the muscles that move the jaw, and the surrounding connective tissues. They commonly cause persistent pain, reduced range of motion, and mechanical symptoms such as clicking, popping, or intermittent locking that go beyond ordinary, short-lived jaw stiffness. Unlike temporary tightness after yawning or chewing, TMJ disorders reflect functional changes in the joint or muscles that may require focused treatment.
These conditions can be acute or chronic and often fluctuate with activity, stress, and sleep habits. A careful evaluation seeks to identify whether symptoms stem from muscle overuse, disc displacement, joint inflammation, or a combination of factors. Early recognition and a targeted plan improve the chances of reducing pain and restoring normal jaw function.
TMJ disorders usually arise from multiple overlapping factors rather than a single cause. Common contributors include teeth grinding or clenching (bruxism), direct trauma to the jaw, repetitive strain from chewing or habits like gum chewing, and structural changes related to arthritis or joint wear.
Certain personal and lifestyle factors increase risk, such as chronic stress, poor posture that affects neck and jaw alignment, and untreated sleep-related breathing problems. TMJ disorders can affect people of any age but are more frequently diagnosed in adults and are reported more often among women for reasons that likely include hormonal and behavioral influences.
Seek an evaluation if you experience ongoing jaw pain or tenderness that interferes with eating, speaking, or daily activities. Other red flags include audible joint sounds like clicks or grating, episodes of jaw locking, limited opening, and persistent muscle fatigue in the face, neck, or shoulders.
Because TMJ problems often produce secondary symptoms, you should also consider assessment for chronic headaches, ear discomfort or fullness, ringing in the ears, or dizziness that accompanies jaw movement. Early assessment helps distinguish TMJ-related complaints from other conditions and guides a treatment plan tailored to the underlying causes.
Evaluation begins with a detailed history and clinical exam to map pain patterns, jaw motion limits, and muscle tenderness. The clinician observes how the teeth come together, listens for joint sounds, palpates muscles of the face and neck, and measures range of motion to identify mechanical restrictions or muscle imbalance.
When indicated, imaging such as cone-beam computed tomography (CBCT) or magnetic resonance imaging (MRI) provides detailed views of bone, joint spaces, and soft tissues to clarify disc position or joint degeneration. At the office of Bella Vida Dental, these diagnostic tools are combined with patient education to create a clear, stepwise plan aimed at restoring comfort and function.
Initial treatment emphasizes conservative, reversible approaches designed to reduce pain and normalize function. This often includes behavioral changes such as avoiding hard or chewy foods, limiting gum chewing, and identifying and modifying parafunctional habits like clenching.
Other commonly recommended strategies include guided jaw-stretching and relaxation exercises, short-term use of over-the-counter anti-inflammatory medication as appropriate, and the use of stabilization splints or night guards to protect teeth and reduce nocturnal clenching. These methods frequently provide meaningful relief and can be combined with physical therapy when muscle imbalance is present.
Night guards, also called occlusal splints, are a common conservative tool for patients who clench or grind their teeth during sleep. A properly fitted device redistributes bite forces, reduces direct stress on the joint and teeth, and can interrupt the cycle of muscle overactivity that contributes to pain.
These appliances are most effective when custom-made from impressions or digital scans to match the patient’s bite and when they are part of a broader management plan that addresses contributing behaviors and muscle tension. Follow-up visits ensure the device fits well and that symptoms are improving, with adjustments made as needed.
Advanced interventions are considered when conservative care has not achieved adequate relief or when imaging identifies specific structural problems that are likely to benefit from targeted procedures. Options may include intra-articular injections, corticosteroid therapy for inflammatory conditions, or selective use of neuromodulators such as Botox® for muscle-related pain in carefully selected cases.
Surgical approaches are reserved for structural abnormalities that do not respond to non-surgical measures and are pursued after multidisciplinary evaluation with detailed imaging and consultations. The decision to escalate care balances potential benefits, risks, and the patient’s functional goals, and it is made collaboratively with the patient and appropriate specialists.
Physical therapy targets muscle balance, posture, and joint mechanics to reduce abnormal stress on the TMJ complex. A trained therapist uses manual techniques, targeted strengthening and stretching exercises, and posture retraining to restore efficient muscle coordination between the jaw, neck, and shoulders.
At-home exercises and self-care techniques complement formal therapy and empower patients to manage flare-ups, improve range of motion, and decrease pain frequency. Consistent practice of prescribed movements and posture habits often produces steady improvement and reduces reliance on passive therapies.
Sleep-related breathing disorders and TMJ dysfunction can be interconnected in several ways, with sleep bruxism (teeth grinding) often occurring alongside obstructive sleep apnea or other sleep disturbances. Repetitive nocturnal clenching places significant load on the jaw and its supporting structures, potentially worsening TMJ symptoms over time.
Addressing sleep issues can therefore be an important part of comprehensive TMJ care, and collaboration between dental and sleep medicine providers helps ensure both conditions are evaluated and managed. Identifying and treating underlying sleep disorders may reduce parafunctional activity and support longer-term relief from TMJ-related pain.
A TMJ evaluation typically begins with a focused history that reviews symptom patterns, dental history, sleep and stress factors, and any prior treatments. The clinical exam includes observation of jaw movement, palpation of muscles, assessment of bite relationships, and documentation of joint sounds and range of motion to identify mechanical or muscular contributors.
If needed, the team will recommend imaging such as CBCT or MRI to visualize joint structures and guide treatment choices. From there, a personalized, evidence-based plan is developed that may combine conservative therapies, referrals to physical therapy or sleep specialists, and periodic follow-up to monitor progress and adjust care as needed.

Ready to schedule your next dental appointment or have questions about our services?
Contacting Bella Vida Dental is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.