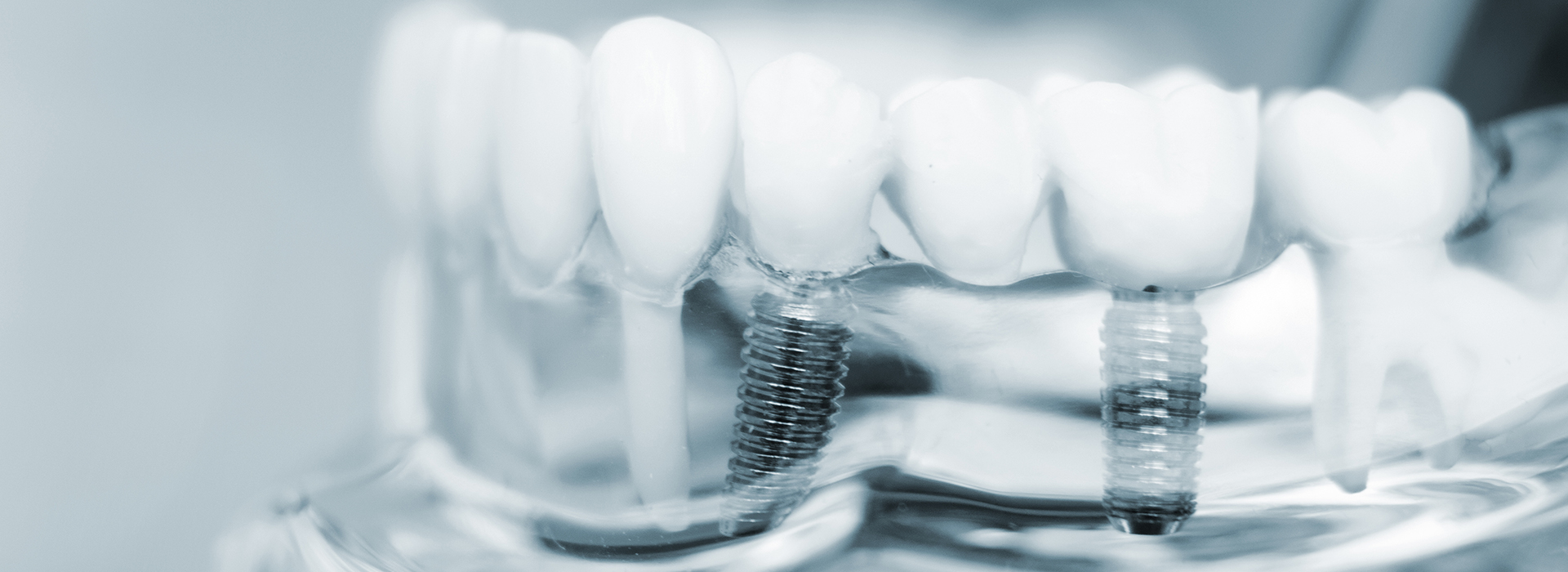
Tooth loss affects many adults and can have consequences beyond appearance — it changes how you chew, how your jaw and facial tissues support one another, and how comfortable you feel when you speak or smile. Today’s dental implants are designed to restore both the visible tooth and the part you don’t see: the root-like anchor that supports lasting function. Because they integrate with the jawbone, implants provide a stable foundation that ordinary removable options cannot match.
When placed with careful planning and appropriate prosthetic design, implants allow patients to eat a wide variety of foods, speak without concern for slipping, and maintain the natural shape of their face. For many people, that combination of stability and natural feel makes implants the preferred long-term approach to replacing one or more teeth. We focus on treatments that aim to return both comfort and confidence, and that protect oral health for years to come.
This page explains how implants work, the different ways they can be used, and what to expect from evaluation through recovery. Our goal is to give you clear, practical information so you can make an informed decision alongside your dentist. If you’d like to discuss options specific to your health and goals, our team at Bella Vida Dental can help you explore the best path forward.

Dental implants are biocompatible posts, typically made of titanium or titanium alloy, that are placed into the jawbone to act as artificial tooth roots. Once an implant fuses with bone through a process called osseointegration, it provides a secure anchor for a crown, bridge, or denture. That secure attachment helps preserve jawbone volume and prevents the collapse of facial tissues that commonly follows tooth loss.
Beyond structural benefits, implants simplify daily life for many patients. They remove the worry of a prosthesis coming loose during meals or conversation, and because they do not rely on adjacent teeth for support, they preserve healthy tooth structure that otherwise might need to be altered for a traditional bridge. With proper oral hygiene and regular dental care, implants are designed to function for many years.
Implant dentistry is a multi-disciplinary field: restorative planning, surgical placement, and prosthetic design all work together. Your dentist will evaluate your bite, gum health, and bone quality, and then collaborate with dental technicians to craft a final restoration that looks and feels natural within your smile.
A single-tooth implant topped with a ceramic crown is often the best option when one tooth is missing. This approach restores a single gap without requiring the adjacent teeth to be shaped or crowned. The result is a self-supporting tooth replacement that closely resembles the size, shade, and alignment of a natural tooth, and one that preserves the health of surrounding teeth.
For patients who prioritize conservation of their remaining dentition, a single implant can be a straightforward and predictable solution. When planned and executed well, the crown on an implant blends seamlessly with neighboring teeth both visually and functionally.
Choosing a crown material and shade is part of the restorative process; your dentist will work with you to select an option that complements your smile while matching functional needs.
When two or more neighboring teeth are missing, an implant-supported bridge replaces the missing units without relying on adjacent natural teeth for support. Instead, strategically placed implants serve as the anchors for multiple replacement crowns. This preserves healthy tooth structure and maintains the stimulation the jawbone needs to remain strong.
Implant-supported bridges can be designed as fixed restorations that stay in place, providing a stable chewing surface and a natural appearance. They are crafted to distribute bite forces efficiently to the implants, which helps protect both the prosthetic and any remaining natural teeth.
For patients missing a full set of teeth, several implant-based options can recreate a complete dental arch. Fixed full-arch restorations use a set number of implants—commonly four or six—to support an entire row of teeth that remains in place. These solutions recreate the feel and function of natural teeth without daily removal.
Alternatively, implant-retained dentures attach to implants for improved stability while remaining removable for hygiene if desired. These overdentures reduce movement, improve chewing efficiency, and enhance speech compared with traditional removable dentures by providing precise attachment points that resist slipping.
Both approaches aim to improve comfort and quality of life, and your dentist will recommend the best option based on your anatomy, oral health, and lifestyle priorities.
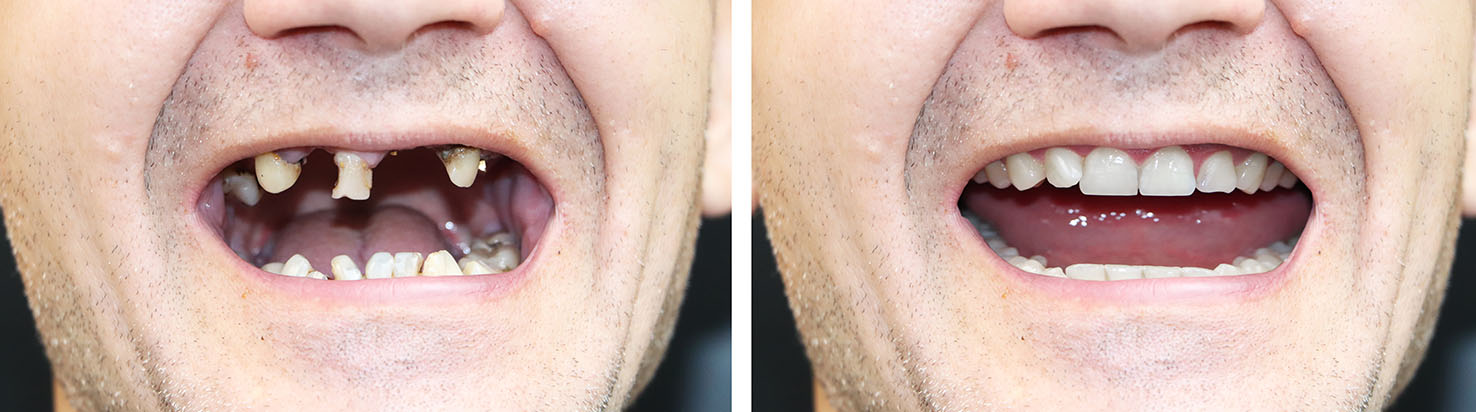
Successful implant care begins with a thorough assessment. This includes a medical and dental history review, a clinical exam, and imaging to evaluate bone quantity and the position of adjacent structures. Digital tools such as 3D imaging help the team plan implant placement with precision and predictability. Treatment planning addresses where implants will be placed, what type of restoration will be used, and whether additional procedures—like bone grafting—are needed to create a stable foundation.
Discussion of anesthesia and comfort options is an important part of planning. Many patients receive local anesthesia and additional sedation if desired, and clear pre- and post-operative instructions are provided to support a smooth recovery.
Implant surgery is typically performed on an outpatient basis and is often well tolerated. The complexity of the appointment depends on how many implants are placed and whether bone grafting or extractions are performed at the same visit. Patients usually experience some soreness and swelling that can be managed with short-term medications and cold compresses; most return to normal activity within a few days to a week.
After placement, implants require a healing period to integrate with the jawbone. For many patients, this takes several months. During that time, temporary restorations can be used to maintain appearance and function. Your dentist will monitor healing and, when appropriate, attach the final prosthesis that is crafted to harmonize with surrounding teeth.
Follow-up appointments and routine dental care remain important after implant placement to help protect soft tissues and the long-term health of the restoration.
Bone loss is a common consequence of tooth extraction or gum disease, and adequate bone volume is essential for stable implant placement. Bone grafting rebuilds lost volume by placing graft material where support is needed so an implant can be anchored securely. Modern grafting techniques are predictable and routinely used when anatomy requires augmentation prior to or at the time of implant placement.
Grafting is planned carefully and tailored to each patient’s needs; the goal is to create a foundation that supports long-term function and natural appearance. Your dentist will explain the grafting process, healing timeline, and how grafts increase the likelihood of a successful implant outcome.
Implants are durable, but like natural teeth they require ongoing care. Regular dental visits, daily hygiene, and protection from excessive forces (for example, night guards for bruxism when needed) all contribute to longevity. When problems do occur—such as prosthetic wear, loosening of a screw, or gum inflammation—early attention typically allows for conservative repairs rather than replacement.
When patients are informed and actively involved in their oral health, implants can deliver years of reliable service and a stable, natural-feeling smile. Your dental team will partner with you to monitor the health of implants and surrounding tissues and to respond proactively whenever maintenance is needed.
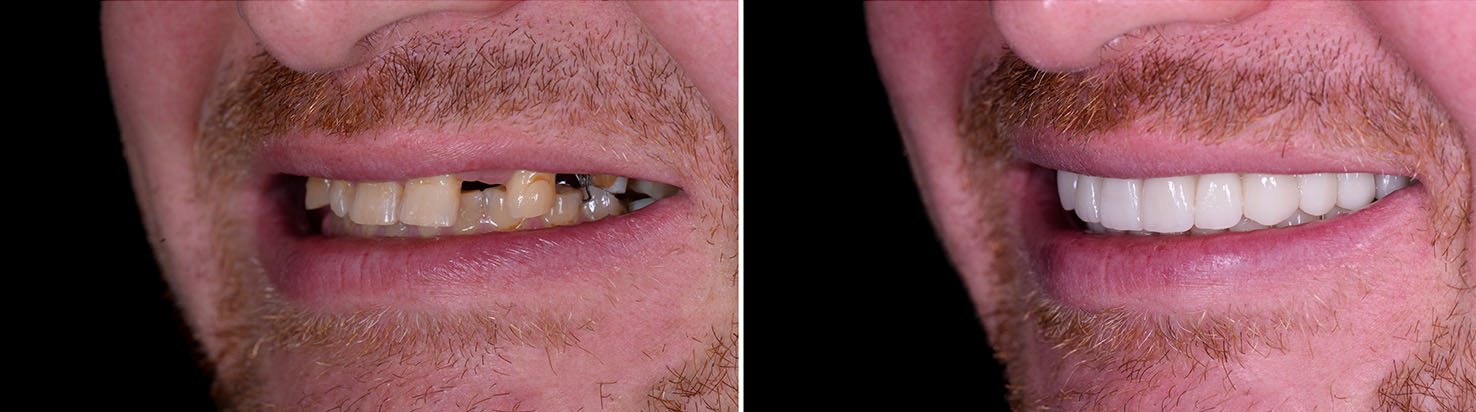
If you’re considering implant dentistry, a consultation with a dental professional will clarify whether implants are appropriate for your situation. The evaluation identifies any preparatory care, outlines treatment options, and sets expectations for timing and outcomes. Patients who move forward do so with a clear plan tailored to their oral health, functional needs, and cosmetic goals.
Our aim is to provide evidence-based recommendations and to guide patients through each stage of care with clear communication and thoughtful follow-through. If you’d like more information about implant dentistry or want to schedule a consultation, please contact us to discuss how we can help you restore a healthy, confident smile.

If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are biocompatible posts, most often made of titanium, that are placed into the jawbone to act as artificial tooth roots. Through a natural process called osseointegration, the implant fuses with bone to provide a stable foundation for a crown, bridge, or denture. The final restoration attaches to the implant and restores chewing function, speech clarity, and the appearance of a natural tooth.
Because implants replace both the visible tooth and the root-like support beneath the gum, they help preserve jawbone volume and maintain facial contours that can change after tooth loss. Implants do not rely on neighboring teeth for support, so they avoid the need to alter adjacent healthy teeth. With proper planning and routine care, implants are designed to provide long-term, reliable tooth replacement.
A good candidate for dental implants is someone who is missing one or more teeth and who has healthy gum tissue and sufficient jawbone to support an implant. General health factors such as controlled systemic conditions, good oral hygiene, and the absence of untreated periodontal disease also influence candidacy. Age alone is not a limiting factor; many adults and older patients successfully receive implants when the supporting tissues are stable.
If bone volume is reduced or medical conditions require attention, treatment planning can often address these issues through bone grafting or medical collaboration before implant placement. A comprehensive evaluation with clinical exams and imaging determines whether implants are appropriate and whether any preparatory procedures are needed. The goal is to create a predictable plan tailored to each patient's anatomy and health history.
Preparation begins with a thorough consultation that includes a review of your medical and dental history, a clinical exam, and imaging such as 3D scans to evaluate bone quantity and anatomical structures. Your dentist will develop a detailed treatment plan outlining the number of implants, the type of restoration, and whether bone grafting or extractions are needed. You will also discuss anesthesia and comfort options so expectations for the appointment are clear.
Before surgery, your team will provide specific preoperative instructions that may include fasting for certain sedation options, temporarily adjusting medications with medical approval, and arranging transportation if sedation is planned. Smoking cessation and good oral hygiene in the days leading up to surgery can improve healing. Clear communication about your health and medications helps reduce risk and supports a smoother surgical experience.
Implant placement is typically performed on an outpatient basis using local anesthesia and, when needed, supplemental sedation to keep you comfortable. The surgeon creates a small opening in the gum to access the jawbone, prepares an implant site with controlled drilling, and places the implant at the planned position and depth. Sutures may be used to close the soft tissue, and a temporary restoration can be provided to protect aesthetics and function during healing when appropriate.
The surgical complexity varies with the number of implants and whether grafting or extractions are done at the same time, but most patients tolerate the procedure well. Over the following weeks to months the implant integrates with bone, at which point an individualized prosthesis is attached and refined for fit and appearance. Regular follow-ups allow the team to monitor healing and complete the restorative phase when integration is sufficient.
Initial recovery commonly involves modest swelling, mild to moderate soreness, and minor bruising around the surgical site; these effects are usually managed with prescribed or over-the-counter medications and cold compresses. Patients are advised to follow a soft diet for a short period and to avoid strenuous activity during the first few days to support healing. Maintaining gentle oral hygiene around the surgical area and attending follow-up appointments helps reduce the risk of complications.
Osseointegration, the process by which the implant bonds with bone, typically takes several months and determines when the final restoration can be attached. Temporary restorations may be used to maintain appearance and basic function during this phase. Contact your dental team if you notice persistent fever, increasing pain, heavy bleeding, or other concerning changes so they can evaluate healing promptly.
For a single missing tooth, a single implant topped with a ceramic crown restores the gap without altering adjacent teeth, providing a self-supporting solution that closely matches the size, shade, and function of a natural tooth. When several adjacent teeth are missing, an implant-supported bridge uses implants as anchors for multiple connected crowns, preserving healthy neighboring teeth and distributing bite forces effectively. These approaches maintain jawbone stimulation and offer a durable alternative to traditional tooth-supported bridges.
For full-arch replacement, options range from fixed restorations supported by a set number of implants to implant-retained overdentures that attach to implants for improved stability while remaining removable for hygiene. Treatment choice depends on oral anatomy, bone availability, and patient lifestyle preferences. Your dental team will recommend the option that best balances function, aesthetics, and long-term maintenance.
Bone grafting is considered when the jaw lacks sufficient volume or density to securely support an implant, a situation that can result from long-term tooth loss, periodontal disease, or trauma. Grafting rebuilds lost bone by placing graft material in the deficient area to create a stable foundation for future implant placement. Materials can include the patient's own bone, donor bone, or synthetic substitutes, and the technique is selected based on the extent and location of the defect.
Grafting can be performed as a separate preparatory procedure or at the time of implant placement, depending on the clinical situation. Healing times vary but often require several months for new bone to mature sufficiently to accept an implant. Proper planning and careful surgical technique make modern bone grafting predictable and increase the likelihood of a successful long-term implant outcome.
Dental implants are designed for long-term function, and many implants last for decades with proper care. Daily oral hygiene, including thorough cleaning around the implant restoration and maintenance of healthy gum tissue, is essential to prevent peri-implant inflammation. Regular dental visits for professional evaluations and cleanings allow your team to monitor implant health and address wear or changes early.
Protective measures such as night guards for patients who grind their teeth and modifications to biting surfaces may extend the life of the restoration. Repairs like tightening a loose screw or replacing a worn crown are often conservative when detected early. Open communication with your dentist and adherence to recommended follow-up schedules help maintain implant stability and function over time.
As with any surgical procedure, implant placement carries risks such as infection, bleeding, and postoperative discomfort, as well as procedure-specific concerns like sinus perforation in the upper jaw or nerve irritation in the lower jaw. Peri-implantitis, an inflammatory condition affecting tissues around implants, can threaten long-term success if not identified and treated early. Thoughtful preoperative assessment, sterile technique, and careful surgical execution reduce the likelihood of these complications.
When complications occur, conservative interventions are preferred whenever possible and may include local treatment of infection, professional debridement, antimicrobial therapy, or prosthetic adjustments. In rare cases, removal and replacement of an implant may be necessary, often following site rehabilitation. Ongoing monitoring and prompt attention to symptoms such as persistent pain, swelling, or mobility improve the chance of preserving the restoration.
Select a provider who demonstrates experience in implant dentistry, uses comprehensive diagnostic tools such as 3D imaging, and offers a coordinated approach to surgical and restorative phases of care. Look for clear communication about treatment planning, timelines, and how the proposed restoration will meet both functional and aesthetic goals. A thorough practice will review your medical history, perform a clinical exam, and explain whether additional procedures like grafting are needed to support a predictable outcome.
At Bella Vida Dental, consultations include personalized evaluations, digital imaging when indicated, and a collaborative discussion of treatment options tailored to your needs and priorities. Expect to receive clear preoperative and postoperative instructions and to have opportunities to ask questions about the procedure, healing process, and long-term care. This preparation supports confident decision making and a smoother treatment experience.

Ready to schedule your next dental appointment or have questions about our services?
Contacting Bella Vida Dental is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.