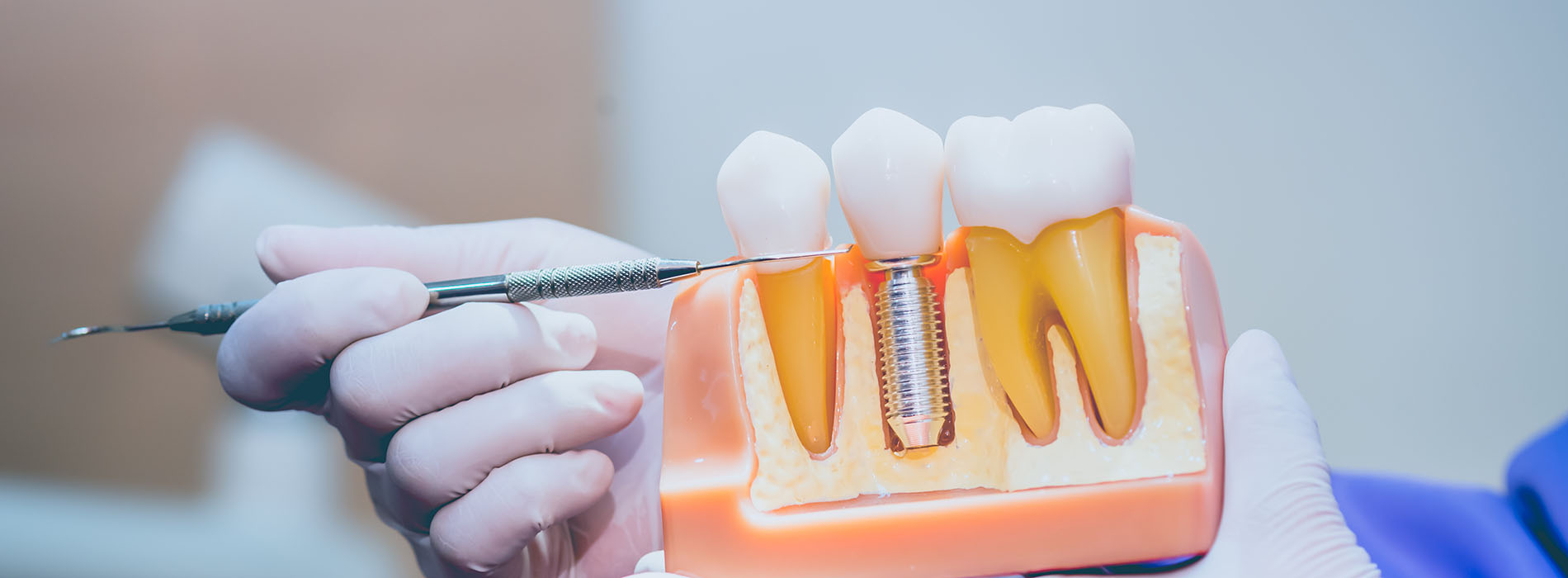
Implant restorations are the visible, functional components that attach to dental implants to replace missing teeth. Unlike removable dentures or traditional bridges that rely on surrounding teeth for support, implant restorations are anchored to titanium posts placed in the jawbone. This creates a stable foundation that mimics the natural tooth root and restores chewing ability, speech clarity, and facial structure.
There are two complementary parts to the process: the implant itself, which integrates with the bone, and the restoration, which is the crown, bridge, or denture you see and use every day. The restoration is carefully shaped and shaded to match neighboring teeth, restore proper bite relationships, and deliver a natural appearance. When designed and placed well, implant restorations can feel and function much like your original teeth.
Understanding the distinction between implant placement and implant restoration helps patients set realistic expectations. Placement is a surgical step focused on establishing a long-term root substitute; restoration is the prosthetic phase that returns full function and esthetics. Both phases require coordination between surgical and restorative teams to achieve predictable, lasting outcomes.
One of the most important benefits of implant-supported restorations is stability. Because the prosthetic is anchored to the bone via the implant, common problems like slipping, clicking, or the need for adhesives associated with removable prosthetics are greatly reduced or eliminated. This reliability makes eating, speaking, and laughing with confidence possible for many patients.
Implants also help preserve jawbone and facial contours. When a natural tooth is lost, the underlying bone begins to resorb over time. An implant transmits functional forces to the bone, stimulating and maintaining its volume — a critical factor in preserving facial structure and preventing the “sunken” appearance that can accompany long-term tooth loss.
From a long-term perspective, implant restorations can protect adjacent teeth and oral health. Unlike traditional bridges that require shaving down healthy teeth for support, implant restorations stand independently. This conservative approach preserves neighboring tooth structure while providing robust chewing function and easier maintenance around individual replacements.
Single-tooth implant crowns replace an individual missing tooth with a customized porcelain crown attached to an implant abutment. These restorations restore the look and function of a single tooth without relying on adjacent teeth for support. They are a predictable option for patients who want a discreet, permanent solution to isolated tooth loss.
For patients missing several adjacent teeth, implant-supported bridges can replace multiple teeth with fewer implants than teeth replaced. These bridges provide strong, unified chewing surfaces and are crafted to blend seamlessly with neighboring natural teeth. They are particularly useful when a gap is too large for a single crown but the patient prefers a fixed restoration over a removable option.
When most or all teeth in an arch need replacement, implant-retained full-arch solutions deliver dramatic functional and aesthetic improvements. Options include implant-supported dentures and hybrid fixed prostheses such as All-on-4® or All-on-6® configurations. These solutions use strategically placed implants to support a full arch of teeth, restoring strong bite force and simplifying daily care compared with traditional dentures.
Intermediate prosthetics, such as overdentures, combine the convenience of removable devices with the retention and stability of implants. Overdentures snap onto locator attachments or bars connected to implants, improving stability while remaining removable for cleaning. The selection among crowns, bridges, overdentures, and full-arch systems depends on bone volume, patient goals, and long-term oral health considerations.
Successful implant restorations begin with comprehensive planning. This typically includes a clinical exam, digital imaging such as CBCT scans, and careful evaluation of bite dynamics and aesthetic goals. Digital planning tools allow the team to map implant positions precisely, anticipate anatomical considerations, and prepare a prosthetic design that will align with your smile and function.
Implant placement is a controlled surgical procedure performed under local anesthesia, with sedation available when appropriate. After the implant is set into the jaw, a healing period follows to allow osseointegration — the biological attachment between bone and implant. Healing times vary by patient and location in the mouth, but modern techniques and careful case selection help optimize outcomes.
Once integration is complete, the restorative phase begins. Impressions or digital scans capture fine details of the implant position, surrounding gum tissue, and opposing dentition. Lab-fabricated crowns, bridges, or hybrid prostheses are designed for precise fit, balanced bite, and natural appearance. Trial fittings ensure occlusion and esthetics are correct before final cementation or screw-retention.
Post-restoration follow-up is part of the process: adjustments to occlusion, periodic monitoring of tissue health, and routine hygiene visits help maintain long-term performance. Clear communication between the restorative team and the patient during each stage ensures predictable results and helps address any concerns promptly.
With proper care, implant restorations can provide many years of reliable service. Daily oral hygiene — including brushing, interdental cleaning, and regular professional cleanings — is essential to keep surrounding gums and bone healthy. Because implants lack a periodontal ligament, periodontal maintenance focuses on preventing plaque accumulation and controlling inflammation around the restoration.
Routine dental visits allow the team to monitor the restoration, check occlusion, and evaluate the condition of the surrounding tissues and bone. If minor adjustments or repairs are needed over time, many restorations are designed to be serviceable; screw-retained prostheses, for example, can be removed for maintenance without disrupting the implant itself. Early detection of potential issues makes corrective care simpler and more predictable.
Expect to work with your dental team to establish a long-term maintenance plan tailored to your situation. Factors such as bruxism, smoking, uncontrolled diabetes, and oral hygiene practices influence both the longevity and maintenance needs of implant restorations. Proactive care and honest communication with your dental providers help maximize lifespan and satisfaction.
The office of Bella Vida Dental combines digital planning, high-quality materials, and an individualized approach to restoration design. Whether you are considering a single crown or a full-arch solution, the team focuses on predictable procedures and ongoing support so you can enjoy the functional and aesthetic benefits of implant restorations for years to come.
In summary, implant restorations are a durable, natural-feeling way to replace missing teeth and protect long-term oral health. Thoughtful planning, careful surgical technique, and meticulous restorative work all contribute to successful outcomes. Contact us to learn more about how implant restorations may fit your needs and to schedule a consultation with our experienced team.

Implant restorations are the visible prosthetic components that attach to dental implants and replace missing teeth. They connect to titanium posts anchored in the jawbone and function as the new tooth structure. This two-part approach—surgical placement of the implant followed by prosthetic restoration—recreates both root support and the chewing surface.
Restorations can be single crowns, bridges, or implant-retained dentures and are shaped and shaded to match adjacent teeth. Properly designed restorations restore bite relationships, speech, and chewing ability while preserving facial contours. When precisely fitted, they can feel and function much like natural teeth.
Implant placement is a surgical procedure focused on inserting a titanium post into the jawbone, while implant restoration is the prosthetic phase that replaces the visible tooth structure. Placement requires careful attention to anatomy and healing, whereas restoration emphasizes fit, occlusion, and esthetics. Understanding this distinction helps set realistic expectations for timing and the sequence of care.
The surgical and restorative teams work together, often using digital planning and CBCT imaging to determine ideal implant positions for final prosthetics. Communication during healing helps guide abutment selection and the design of crowns, bridges, or dentures. Patients should expect staged appointments and clear explanations of each phase before moving forward.
Single-tooth crowns attach to individual implants to replace isolated tooth loss and preserve neighboring teeth. Implant-supported bridges can span multiple missing teeth and use fewer implants than the number of teeth replaced. Overdentures use attachments or bars to improve stability while remaining removable for cleaning. Each option balances retention, hygiene access, and patient preferences for fixed versus removable solutions.
Full-arch solutions such as All-on-4® or All-on-6® use strategically placed implants to support a fixed prosthesis or a hybrid denture when most teeth in an arch are missing. Hybrid fixed prostheses combine a rigid framework with layered esthetic materials to restore strong bite force and natural appearance. Your clinician will recommend the best solution based on available bone, esthetic goals, and long-term maintenance needs.
Good candidates for implant restorations generally have adequate jawbone volume, controlled systemic health, and a commitment to oral hygiene. Smoking, uncontrolled diabetes, and active periodontal disease can increase risk and may require management before treatment. Younger patients whose jaws are still growing are usually not ideal candidates. A clinical exam and imaging determine whether local or systemic factors need to be addressed to proceed safely.
Bone grafting, sinus lifts, and staged approaches can extend implant options to patients with reduced bone volume, making restoration possible for many who initially appear ineligible. Digital CBCT scans and careful treatment planning clarify the need for augmentation and the anticipated timeline for healing. At Bella Vida Dental, the team evaluates each case individually to tailor a restorative pathway that aligns with the patient’s goals and oral health status.
The treatment timeline begins with diagnostics and planning, including a clinical exam, digital imaging, and occlusal analysis. Implant placement is then performed under local anesthesia with sedation options available for patient comfort. A healing period follows to allow osseointegration, and the duration varies by location, bone quality, and individual healing capacity.
After integration, the restorative phase involves digital scans or impressions, lab fabrication, and trial fittings before final placement. Patients typically return for occlusal adjustments and follow-up checks to ensure comfort and function. Clear communication about milestones helps patients anticipate the sequence and timing of visits.
Common restorative materials include zirconia, porcelain-fused-to-metal, and layered ceramic systems, each offering a balance of strength and esthetics. Titanium or ceramic abutments provide the substructure that connects the restoration to the implant and influence tissue response. Material choice depends on the location of the restoration, bite forces, and desired translucency for a natural appearance.
High-quality lab fabrication and meticulous shade matching are essential to achieve a seamless integration with neighboring teeth. In some cases, a stronger substructure is chosen in posterior regions while more translucent ceramics are used in the smile zone for lifelike results. Your clinician will discuss material advantages and trade-offs during the restorative planning appointment.
Daily care for implant restorations follows many of the same principles as natural teeth: thorough brushing and regular interdental cleaning to control plaque and inflammation. Specialized tools such as interdental brushes, floss designed for implants, or water flossers can improve access around abutments and prosthetic margins. Good home care reduces the risk of peri-implantitis and helps maintain healthy soft tissues around the restoration.
Professional maintenance visits include soft-tissue assessment, professional cleaning with implant-safe instruments, and occlusal checks to identify wear or loosening early. If bruxism or other parafunctional habits are present, nightguards or occlusal adjustments may be recommended to protect the restoration. A collaborative maintenance plan between patient and clinician supports long-term performance.
With proper care, implant restorations often last many years and sometimes decades, while the implant fixture itself can remain stable long-term. Prosthetic components can experience normal wear and may require repair or replacement over time, depending on material and function. Routine monitoring allows clinicians to address small problems before they become major complications.
Factors that influence longevity include oral hygiene, smoking status, systemic health conditions, bruxism, and the quality of the initial restorative design. Regular dental visits and adherence to recommended maintenance protocols improve outcomes and reduce the likelihood of failure. Early intervention for signs of tissue changes or mechanical issues preserves both implants and prosthetics.
Possible complications include peri-implant mucositis and peri-implantitis, mechanical loosening of screws, and prosthetic fractures; early recognition is important. Symptoms such as persistent redness, swelling, bleeding on probing, or mobility warrant prompt clinical evaluation. Risk mitigation includes meticulous hygiene, appropriate material selection, and careful occlusal management.
When complications arise, treatments range from non-surgical cleaning and localized therapy to prosthetic repair or, in rare cases, surgical intervention to manage advanced infection. A coordinated approach between surgical and restorative clinicians helps determine the least invasive and most predictable solution. Patient education on signs to watch for expedites care and improves the chance of preserving the implant and restoration.
Modern restorative planning commonly uses CBCT imaging, intraoral scanning, and digital workflows to design implant positions and prosthetic contours before surgery. This digital coordination improves the accuracy of implant placement and reduces surprises during the restorative phase. Close collaboration with dental laboratories ensures that the final prosthesis meets functional and esthetic objectives.
The office of Bella Vida Dental combines digital planning, high-quality materials, and individualized restorative protocols to deliver predictable results and ongoing support. Patients receive clear instructions for preoperative preparation, postoperative care, and long-term maintenance tailored to their restoration. That multidisciplinary, patient-centered approach helps safeguard outcomes and maintain oral health for years to come.

Ready to schedule your next dental appointment or have questions about our services?
Contacting Bella Vida Dental is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.