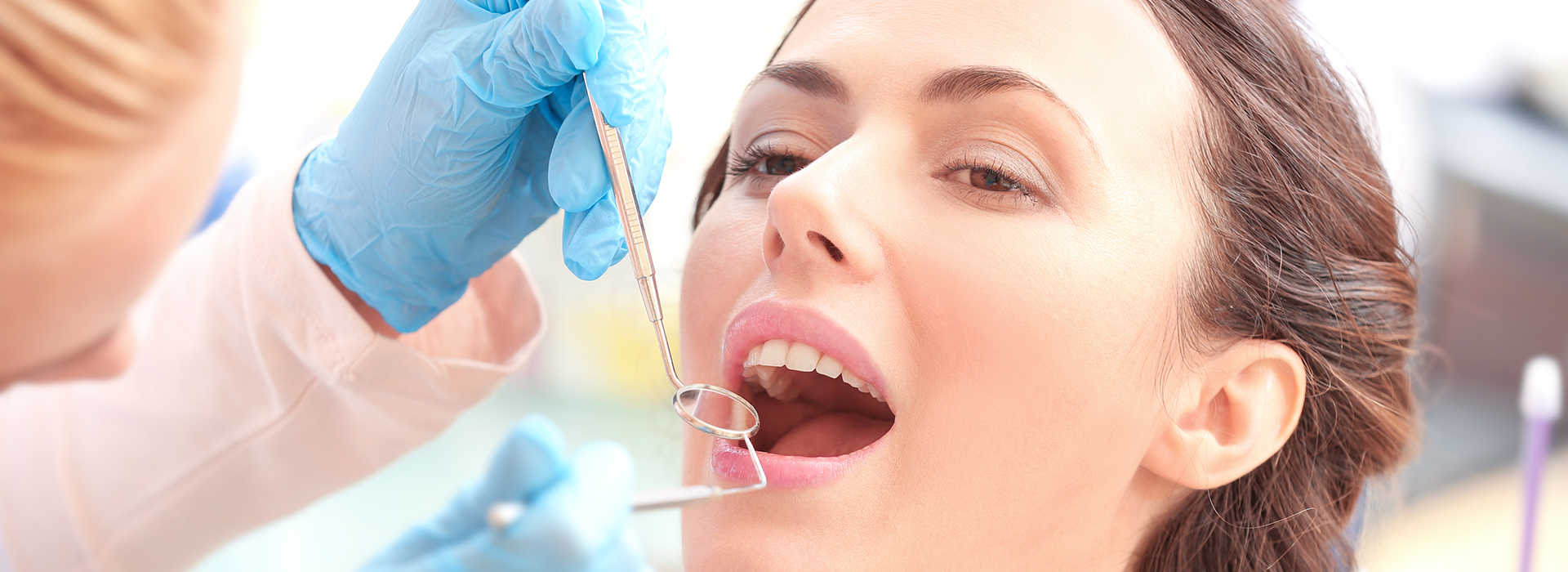
Gum disease is the leading reason adults lose teeth, and it affects a large portion of the population: roughly half of adults over 30 show some form of periodontal disease. The condition ranges from mild inflammation to progressive destruction of the tissues that anchor teeth in the jaw. At the office of Bella Vida Dental, we provide thorough periodontal care designed to identify problems early, preserve natural teeth whenever possible, and restore oral health with techniques backed by current dental science.
Periodontal disease starts at the surface: bacteria in dental plaque irritate the gum tissue and trigger inflammation. Over time, if plaque and calculus (tartar) are not removed, the inflammatory response can damage the soft tissues and the underlying bone that support teeth. Because early stages are often painless, many people are surprised to learn they have a problem only after significant change has occurred.
Routinely brushing and flossing disrupts the bacterial film that causes inflammation, but even with diligent home care, tartar can accumulate out of reach of a toothbrush. That is why professional assessment and cleaning are essential—these visits let clinicians measure pocket depths, examine gum attachment, and detect changes that the patient might not feel yet.
Recognizing the common warning signs helps catch disease while it’s still manageable. Pay attention to symptoms and share them with your dental team so that a timely plan can be put in place to protect your smile.
Signs to watch for include:
Red, swollen, or tender gum tissue
Bleeding during brushing or flossing
Gum recession or roots becoming exposed
Persistent bad breath or an unpleasant taste
Loose teeth, shifting contacts, or new gaps

Healthy gums do more than support your smile—they play a role in your overall health. Research continues to show associations between chronic periodontal inflammation and systemic conditions such as diabetes, cardiovascular disease, and respiratory illnesses. While the nature of these links is complex, reducing oral inflammation is a practical step toward lowering the burden of chronic disease.
Prevention and early intervention are the most effective strategies. Regular exams and cleanings let clinicians detect subtle changes in gum health and respond before damage becomes extensive. Our approach emphasizes straightforward steps you can take to reduce risk and maintain a more stable oral environment over time.
At Bella Vida Dental, we aim to partner with patients to create care plans that respect individual health histories and lifestyle factors. That collaborative process makes it easier to achieve lasting results and helps protect both oral and general health.
The earliest stage of gum disease—gingivitis—is marked by inflammation confined to the soft tissue. At this point, the underlying bone is still intact and the condition is typically reversible. Symptoms often include bleeding with brushing, redness, and slight swelling. Because discomfort is usually minimal, gingivitis commonly goes untreated until a routine exam brings it to light.
Addressing gingivitis centers on improved plaque control and professional cleaning. A focused hygiene routine, combined with one or more deeper cleanings, can remove the irritants that drive inflammation and allow tissues to heal. For many patients, committed home care plus periodic maintenance prevents recurrence and restores healthy gum tone.
When lifestyle factors—such as smoking, uncontrolled diabetes, or inconsistent oral hygiene—are present, clinicians will discuss targeted strategies to improve response to treatment. The goal at this stage is simple: eliminate active inflammation and keep it from returning.

If inflammation persists, it can progress from gingivitis to periodontitis, a stage in which the connective tissues and the jawbone that hold teeth begin to break down. This process increases pocket depths around teeth, causes roots to become exposed, and, in time, can lead to tooth mobility or loss. Because bone and attachment do not regenerate spontaneously, timely intervention is crucial.
Treatment for periodontitis aims to stop destructive processes and preserve as much natural support as possible. Clinicians evaluate the pattern and severity of tissue loss, measure pocket depths, and look for areas of bone loss on radiographs. From that assessment, a stepwise plan is developed to control infection and rebuild a safer foundation for the dentition.
Modern periodontal therapy includes both non-surgical and surgical options. Advances in materials and regenerative techniques mean many patients can receive care tailored to their needs, with an emphasis on function, stability, and a more natural appearance of the gums and teeth.
A dental team begins periodontal care with a comprehensive exam that includes clinical measurements and imaging as needed. Probing depths, bleeding on probing, level of attachment, and radiographic bone height are recorded to determine the disease stage and guide treatment priorities. This diagnostic snapshot allows providers to recommend an evidence-based sequence of care.
Every treatment plan is individualized. Factors such as the extent of pocketing, medical history, smoking status, and patient goals influence choices between conservative measures and more invasive interventions. Clinicians also discuss realistic expectations and the maintenance steps needed to protect long-term outcomes.
We use a combination of therapies to reduce bacterial load, control inflammation, and, where appropriate, encourage tissue regeneration. Your dental provider will explain each option, why it is recommended, and how it fits into an overall maintenance strategy designed to keep disease at bay.
Early and moderate disease is often managed without surgery. Scaling and root planing (deep cleaning) removes plaque and calculus from below the gumline and smooths root surfaces so healing can occur. These procedures reduce pocket depths and make it easier for patients to maintain healthy gums at home.
Adjunctive therapies—such as localized antimicrobials placed into pockets or prescribed systemic antibiotics when indicated—can help lower bacterial levels during healing. In addition, clinicians may recommend more frequent maintenance visits to monitor response and prevent recurrence.
The intent of conservative care is to restore a stable environment where routine hygiene is effective and further tissue breakdown is halted. When this approach succeeds, many patients enjoy long stretches of periodontal health with minimal intervention.
When pocket depths and bone loss are beyond the reach of non-surgical techniques, surgical treatment can access and clean affected root surfaces and reshape supporting tissues. Procedures such as flap surgery allow precise removal of diseased tissue and improved access for thorough debridement.
Where tissue and bone have been lost, regenerative methods—bone grafts, guided tissue regeneration, and biologic agents—may be used to encourage new attachment and restore support. These procedures are selected based on the specific defects and the patient's overall health status.
Contemporary tools, including dental lasers in select cases, provide additional options for reducing pocket depths, treating inflammation around implants, and refining gum contours for improved function and esthetics. As always, surgical care is paired with a long-term maintenance plan to protect the investment of treatment.
Keeping periodontal disease under control is a collaborative process that combines professional care, effective home hygiene, and regular monitoring. If you have concerns about bleeding gums, loose teeth, or changes in your bite, contact us for more information about periodontal evaluation and treatment options.

Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
At the office of Bella Vida Dental, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.
Periodontal treatment refers to the range of professional therapies used to prevent, control, and repair disease of the gums and the bone that support teeth. These therapies address conditions from reversible gingivitis to advanced periodontitis and may include non-surgical care, surgical procedures, and maintenance protocols. The primary goals are to stop infection, preserve natural tooth support, and restore a healthy oral environment for long-term function.
Care is individualized based on the extent of tissue and bone involvement, the patient’s systemic health, and oral hygiene habits. Treatment often begins with diagnostic measurements and imaging to map areas of pocketing and bone loss, then proceeds through a stepwise plan tailored to those findings. At Bella Vida Dental in Tucson, AZ, clinicians emphasize evidence-based approaches and ongoing monitoring to protect each patient’s oral health.
Gum disease typically begins when dental plaque, a bacteria-rich film, accumulates along the gumline and provokes an inflammatory response in the soft tissue. Early inflammation, or gingivitis, often produces minimal discomfort, so many people do not recognize the problem until a dental exam reveals changes in pocket depths or attachment. Without removal of plaque and calculus, the inflammatory process can progress and damage the connective tissue and bone that anchor teeth.
Routine home care reduces bacterial load, but tartar can form below the gumline where a toothbrush cannot reach, making professional assessment essential. Clinicians use probing and radiographs to detect hidden disease and to document progression before symptoms like pain or loose teeth appear. Catching issues early improves the likelihood that simple therapies will restore health and prevent extensive tissue loss.
Common warning signs include gums that are red, swollen, or tender and bleeding during brushing or flossing, which indicate active inflammation. Other signs may be persistent bad breath, a noticeable change in how teeth fit together, gum recession with exposed roots, or teeth that feel mobile. These symptoms can vary in intensity and may not appear in early stages, underscoring the value of routine periodontal screening.
If you notice any of these changes, report them to your dental provider so a timely evaluation can be scheduled. Early identification allows clinicians to recommend targeted therapies and maintenance plans that limit progression and preserve oral function. Monitoring over time also helps assess how well treatment is working and when additional interventions are needed.
Diagnosis begins with a comprehensive clinical exam that measures pocket depths, assesses bleeding on probing, and evaluates levels of attachment around each tooth. Dental radiographs or CBCT imaging are used to reveal the pattern and amount of bone loss, and a review of medical history and habits such as smoking or diabetes status helps contextualize risk. Together these data points determine the disease stage and inform a personalized treatment sequence.
Accurate documentation at the initial visit creates a baseline for tracking response to therapy and for planning maintenance intervals. In some cases clinicians may also take microbial or genetic tests to guide adjunctive therapies, though the core assessment remains probing and imaging. Clear communication about findings and realistic expectations is an important part of the diagnostic visit.
Non-surgical care is often the first line of treatment and includes procedures such as scaling and root planing to remove plaque and calculus from beneath the gumline and to smooth root surfaces. These deep cleanings reduce pocket depths, lower bacterial load, and create an environment that supports tissue reattachment and healing. Clinicians may also use localized antimicrobials or recommend systemic antibiotics when indicated to help control infection during the healing phase.
Following active therapy, most patients enter a periodontal maintenance program with more frequent professional cleanings and monitoring to prevent recurrence. Home-care improvements—effective brushing, interdental cleaning, and risk-factor management like smoking cessation—are essential for long-term success. When non-surgical measures achieve stable tissue levels, many patients can maintain health with conservative care and periodic review.
Surgical and regenerative therapies are considered when non-surgical treatment cannot adequately access deep pockets or when bone and attachment loss is significant. Procedures such as flap surgery permit direct visualization and thorough cleaning of root surfaces, while regenerative techniques like bone grafting and guided tissue regeneration aim to rebuild lost support in specific defects. The decision to proceed surgically is based on the pattern of bone loss, patient health, and the likelihood that regenerative methods will improve long-term prognosis.
Contemporary surgical care may also incorporate biologic agents and, in select cases, dental lasers to reduce inflammation and refine soft tissue contours. Postoperative maintenance and excellent home care remain critical to protecting any surgical gains in tissue attachment. Clinicians discuss expected outcomes, risks, and the maintenance commitment required to preserve results before moving forward with operative care.
Effective home care begins with consistent twice-daily brushing using a technique that gently cleans along the gumline, complemented by daily interdental cleaning with floss or interdental brushes. For many patients, adjunctive products such as antimicrobial rinses or prescription gels are recommended temporarily to help control bacterial levels as tissues heal. Tobacco cessation and control of systemic conditions like diabetes are equally important because they directly affect healing and susceptibility to reinfection.
After professional therapy, follow-up visits and a personalized maintenance schedule help reinforce home-care habits and allow clinicians to catch any signs of recurrence early. Keeping scheduled maintenance cleanings and periodontal reassessments ensures that small problems are treated before they become major concerns. Open communication with your dental team about challenges or changes in symptoms will help them adjust strategies to support long-term gum health.
Research shows consistent associations between chronic periodontal inflammation and systemic conditions such as diabetes, cardiovascular disease, and respiratory illnesses, although the relationships are complex and not purely causal. Reducing oral inflammation is a practical step that may lower systemic inflammatory burden and support better control of certain medical conditions, particularly diabetes. Dental providers coordinate with medical teams when systemic health factors are likely to influence periodontal treatment and outcomes.
Maintaining periodontal health is therefore important not only for preserving teeth but also for supporting broader health goals. Regular periodontal care and management of risk factors like smoking and uncontrolled blood sugar contribute to both oral and general well-being. Patients should inform their dental team about medical diagnoses and medications so care can be adapted accordingly.
Dental implants require the same careful attention to surrounding soft tissue and bone as natural teeth, but the biology differs and implants can develop peri-implant mucositis or peri-implantitis when inflammation is not controlled. Early-stage soft tissue inflammation around an implant is often reversible with professional cleaning and improved hygiene, while advanced peri-implant bone loss may require surgical intervention and regenerative techniques tailored to the implant site. Clinicians evaluate implant health with probing, radiographs, and clinical inspection to determine the appropriate course of action.
Maintenance of implants focuses on plaque control, regular professional debridement with instruments safe for implant surfaces, and close monitoring for changes in pocketing or mobility. Patients with implants are often placed on a more frequent recall schedule to catch problems early and preserve the longevity of the restoration. Education about proper cleaning tools and techniques for implants helps reduce the risk of future complications.
You should schedule a periodontal evaluation if you notice bleeding gums, persistent bad breath, gum recession, loose teeth, or changes in how your bite feels, and you should also attend routine exams even when symptoms are absent. At the initial visit the dental team will review your medical history, perform a thorough periodontal exam including probing and charting, and take radiographs or other imaging as needed to assess bone levels. This information is used to stage the disease and to create a personalized treatment plan that addresses immediate needs and long-term maintenance.
The first visit also includes a discussion of risk factors and practical steps you can take at home to support healing, and clinicians will outline recommended next steps whether conservative therapy or specialist referral is indicated. If you have concerns about your gums or have noticed changes in oral health, contact Bella Vida Dental to arrange an evaluation and to learn about the evidence-based options available. Clear communication about expectations and follow-up is part of every treatment journey.

Ready to schedule your next dental appointment or have questions about our services?
Contacting Bella Vida Dental is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.